Bowel Leakage
Make an Appointment
For the Charlottesville area:
For Culpeper:
Fecal incontinence or bowel leakage is the inability to control passage of liquid or solid stool. This condition affects 2-15% of all adults in the United States.
Types of Fecal Incontinence
- Double incontinence: the inability to control both the passage of stool and urine.
- Fecal incontinence: the inability to control the passage of liquid or solid stool.
- Flatal incontinence: the inability to control the passage of gas.
- Rectovaginal fistula: when a connection develops between the vagina and rectum and results in stool being passed uncontrollably through the vagina.
There are many causes of incontinence.
Birth Trauma & Injury
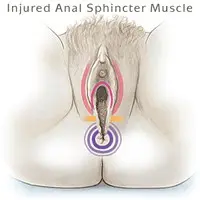
During a difficult vaginal delivery or a delivery that requires use of forceps, vacuum or episiotomy, a partial tear in the anal sphincter muscles can happen. If this chronic third/fourth degree laceration doesn’t heal properly, it can cause incontinence. This tear may also cause a rectovaginal fistula and cause stool to pass from the rectum into the vagina.
Age
Aging has the greatest impact on bowel control in women over the age of 40.
Surgical
Certain surgeries place you at risk for developing fecal incontinence. Most of these surgeries involve pelvis muscles or the sphincter itself. They include:
- Fistulectomy
- Internal sphincterotomy
- Low anterior resection
Diarrheal States
Chronic diarrhea can cause fecal incontinence. Inflammatory bowel disease can cause alternating constipation and diarrhea. Often, if you can control diarrhea with medication or dietary changes, they can also help improve your bowel control.
Laxative Abuse
Laxatives containing Senna can damage your bowels and cause incontinence.
Infectious Enteritis
A virus or bacteria causes this temporary condition. Treatment with antibiotics often improves your bowel control.
Neurological Conditions
Some diseases affect the nerves in the pelvis that help you control bowel movements. You may experience fecal incontinence if these nerves are damaged.
Diseases that can cause nerve damage include:
- Multiple sclerosis
- Parkinson’s disease
- Spinal cord injury
- Stroke
- Dementia
- Diabetic neuropathy
Diagnosing Fecal Incontinence
Your doctor will ask for your health history and ask you some questions.
Pelvic Exam
A pelvic exam helps your doctor check the strength of your rectum muscles and your ability to squeeze those muscles. It also helps to see how well your pelvic organs are supported. Your doctor may perform a digital exam of your rectum and anus to look for hemorrhoids and prior scarring.
Transanal Ultrasound
Your doctor places a finger-size probe into your rectum. The ultrasound allows your doctor to see the anal sphincter, which is the muscle that allows you to control your bowel movements.
MRI
This radiology test allows your doctor to look at your pelvic floor muscles, which help you to control your bowel movements. An MRI also looks at the nerves in your back, which are important for bowel control.
Defecography
This X-ray test allows your doctor to see what happens during a bowel movement and if there are blockages or pelvic organ prolapse. Your doctor places barium paste into your rectum and vagina for this exam.
Anal Manometry
This test allows your doctor to see if your rectum muscles are strong and able to function properly. Your doctor inserts a small air-filled balloon into your rectum, which allows your doctor to determine if the muscles react properly to different pressures.
Treatment For Fecal Incontinence
UVA offers a number of treatment options.
Physical Therapy
- Biofeedback therapy uses a machine to show how your muscles work and how to coordinate them with a full bowel to improve control. Biofeedback can teach you how to empty the bowel effectively while improving your symptoms.
- Electrical Stimulation can help strengthen your muscles. You can either purchase or rent one of these devices to use at home.
- Physical therapists can teach you how to perform pelvic floor muscle contractions (kegel exercises), to strengthen and retrain the pelvic and sphincter muscles. This can help prevent urine or stool leakage when coughing, sneezing or lifting objects. Other benefits include: enhanced sexual function, conditioned muscles to make childbirth easier, decrease and/or prevention of pelvic organ prolapse and improvement in your ability to pass stool.
Surgery
Anal sphincteroplasty repairs injured or separated sphincter muscles. Your doctor makes an opening in the skin between the vagina and anus to stitch together the separated muscles.
Rectovaginal fistula is a procedure where your doctor separates the tract that connects the vagina and rectum with multiple tissue layers. Your doctor makes an incision either between the vagina and anus or just inside the vagina.
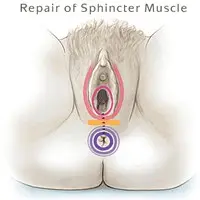
A seton is a ribbon of material (thread, wire, rubber or medicated suture) that your doctor places in a fistula to help you heal. A seton drains the fistula tract to prevent bacteria from collecting and eroding into your tissues. Drainage allows the infection to pass so your doctor can operate at the site of the problem.